MASKS HARBOUR HARMFUL FUNGUS AND BACTERIA
From JC
A new study published yesterday in Scientific Reports titled, “Bacterial And Fungal Isolation From Face Masks Under the COVID-19 Pandemic.”
Uh-oh!
The researchers surveyed 109 medical-school volunteers on their mask usage and lifestyles, and then cultured bacteria and fungi from the face-side and the outer-side of their masks. This will shock you, but they found bacteria and fungi growing on the masks.
Bacterial colonies were found on 99% of the samples on the face-side, and 94% on the outer-side. The researchers found fungal colonies growing on 79% of the samples on the face-side, and 95% on the outer-side. They also found that longer mask usage significantly increased the fungal colony figures (but not the bacterial colony numbers).
Although most of the bacteria were non-pathogenic, they found several potentially pathogenic bugs: S. aureus (commensal bacterium; its overgrowth can cause various diseases); B. cereus (intestinal bacterium, causing food poisoning); Staphylococcus saprophyticus (urinary tract infection); and Pseudomonas luteola (an opportunistic pathogen).
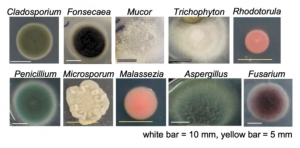
The researchers detected several types of fungus:
The conclusion? The authors suggested “that immunocompromised people should avoid repeated use of masks to prevent microbial infection.”
Haha! Thanks experts! Immunocompromised people are the ones the experts always say should wear masks the most — all the time, if they can. Can you believe by giving that advice the experts were actually setting immunocompromised people up for even worse infections? So which is it? Should immunocompromised people wear masks or not?
What would we do without experts?
Here is what YOU are breathing directly into your Lungs when wearing a Face Diaper
WBOY ran a story last week headlined, “Antimicrobial-Resistant Infections Up 15% During COVID, CDC says.” Tell me it isn’t so.
Antimicrobial resistance is when bacteria and fungus become resistant to antibiotics, antifungals and other treatments. The CDC published its special report last week titled, “COVID-19: U.S. Impact on Antimicrobial Resistance, Special Report 2022.” The special report concludes that the threat of antimicrobial-resistant infections has significantly increased since March 2020, with resistant hospital-onset infections AND DEATHS jumping +15% or more during the first year of the pandemic.
Some resistant bug strains increased a whole lot more than +15%. Carbapenem-resistant Acinetobacter saw a +78% increase, and multidrug-resistant Pseudomonas aeruginosa saw a +32% increase. Also up were Enterococcus (+14%) and Staphylococcus aureus, otherwise known as Mersa (MRSA) (+13%).
Now consider this odd fact: In its 2019 special report, the CDC said that antimicrobial-resistant infections had fallen by -27% during the entire period between 2012 to 2017. But the trend suddenly reversed in March 2020, for some reason.
It can’t have anything to do with the masks, can it? Just asking.
Did these masked marvels never wonder why we swirl mouthwash after brushing our teeth?